How Cooperatives Are Driving the New Economy: In Depth
- Don’t Like Your Health Insurance? Make Your Own
- Share

Photo courtesy of Mercy Health.
Don’t Like Your Health Insurance? Make Your Own
The Affordable Care Act hopes to drive expansion of health care co-ops.
Millions of Americans lack adequate health care, using emergency rooms as a costly alternative or getting no care at all. The Patient Protection and Affordable Care Act (ACA), often called “Obamacare,” opened the door for an affordable option. The December 31, 2012 deal between Congress and the administration that avoided the so-called “fiscal cliff” has, at least for the moment, closed that door for 26 states.
ACA loans for health care cooperatives
The ACA funds private, nonprofit health insurers called Consumer Operated and Oriented Plans—CO-OPs. It originally set aside $3.4 billion for low-interest loans—seed money for at least one health cooperative in each state, plus Washington, D.C.
“Start-up loans” cover such development costs as renting office space, developing provider networks or obtaining contracts with existing provider groups, hiring managers, educating members on how co-ops work, and building enrollment. ACA “solvency loans” are intended to help CO-OPs satisfy state monetary reserve requirements for health insurers.
According to the Center for Medicare Services, CO-OP loans could fund cooperatives that operate health care facilities or cooperative insurance that would cover treatment at participating medical organizations.
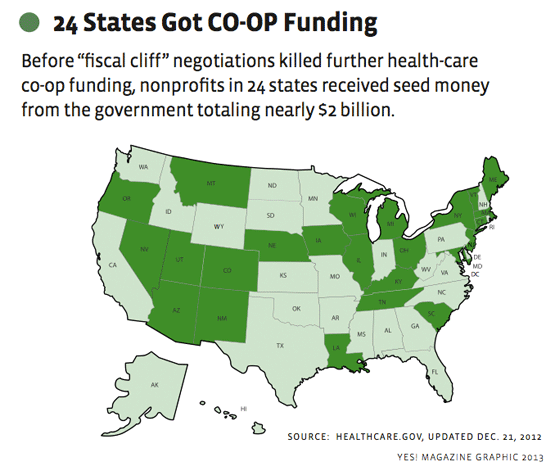
Interest in CO-OPs has been keen. The healthcare.gov website states that, as of December 21, 2012, 24 nonprofits offering coverage in 24 states have been awarded nearly $2 billion.
One of those is the Colorado Health Insurance Cooperative, which received a $69 million ACA grant. “Our state does have a long history of supporting agricultural co-ops to receive better deals and services,” CEO Julie Hutchins says. In fact, the Rocky Mountain Farmers Union, founded in 1907, sponsors the new CO-OP.
“The CO-OP will be a unique option for the thousands of newly insured Coloradans that will flood the market in 2014,” says Hutchins. “We also hope to be a resource for rural Coloradans to access better coverage as these areas of the state have been left with few options in recent years.” She expects a minimum of 8,000 people to join the CO-OP in its first year.
Why create CO-OPs?
Health care CO-OPs are not your usual health insurance companies. The National Cooperative Business Association (NCBA) says, “Cooperatives are owned and democratically controlled by their members … not by outside investors.” Health care cooperatives use the money that a private insurer would take as profit to lower premiums, expand benefits, or improve the quality of care for their members.
In the medical cooperative model, members are active in the decision-making process, from setting policy to electing, and even sitting on, the board of directors. Group Health Cooperative (GHC), established in 1946 in Washington state, involves consumers in committees, advocacy caucuses, forums, and focus groups. Through GHC’s member website, patients have better access to their doctors and their personal medical records. The organization’s longevity is a strong indication that this model, with its emphasis on consumer engagement, is viable in the long run.
That conclusion is borne out by the success of other cooperatives as well. The National Alliance of State Health Cooperatives (NASHCO) points out that “Member ownership [in cooperatives] has worked to serve millions of working families with electrical, telephone, food, farm, and financial services.”
Infusing the Market with Real Choice
Michael Booth of the Denver Post reports that CO-OPs receiving ACA grants are “meant to compete with private insurers and bureaucratic nonprofits, adding a consumer-focused policy to the state health benefits exchanges.” These insurance exchanges go live in January 2014. Functioning as online marketplaces, they will contain information (and phone assistance) on health care plans available to individuals, families, and businesses with 100 or fewer employees. The public can also discuss plans with informed insurance brokers. An estimated 19 million previously uninsured Americans will use these insurance exchanges in 2014 to buy health coverage, increasing to 30 million by 2022.
ACA CO-OP funding will continue in the 24 states where CO-OPs have already been approved in 2012. But, because of the “fiscal cliff” deal, funds have been cut for the additional 26 states still applying for capital loans. NASHCO has fast-tracked their lobbying efforts and is already advocating for the restoration of original ACA CO-OP funding levels.
Perhaps, as the new CO-OPs become operational, they will demonstrate the value of this form of health care and lead to reinstatement of funding for all states, if that has not been accomplished by the time the funded CO-OPs go live.


