News Based on facts, either observed and verified directly by the reporter, or reported and verified from knowledgeable sources.
How to Get Nurses Back in Homes Supporting Disabled Children

Analicia Brokloff just wanted to take her daughter home. Her 2-year-old, Mila, was ready to be discharged from UC Davis Children’s Hospital in Sacramento after having a lung infection.
Mila, who has cerebral palsy, still required the care of a home nurse, as she recovered last fall from having a tracheotomy—a surgical opening in the throat to help her breath.
But no home nurses were available. So, due to staffing shortages and cracks in the health care system—but not due to medical need—Mila had to stay in the hospital. It had been two weeks since she was well enough to go home. She’d arrived in the hospital close to two months ago, and her family and the hospital discharge planner had been searching for a home nurse the whole time.
“It was just really hard,” said Brokloff. “It feels like [children with disabilities] and their parents are falling through the cracks.”
Finding nurses to care for medically fragile children at home has historically been difficult. But since the start of the COVID-19 pandemic, the problem has worsened dramatically, according to parents of children with disabilities and home health agencies. The pandemic set off a surge in demand for nurses at hospitals, clinics, and other health care facilities, and widened the compensation gap between these and lower-paid home nursing jobs. This pulled nurses away from home care. At the same time, large numbers of nurses left the profession—many due to health concerns, retirement, and burnout—shrinking the overall workforce. As a result, fulfilling requests for home nurses has become close to impossible, those in the field said. That’s especially true for the more than 1 in 4 California children with special health care needs who, like Mila, are insured through the state’s public health insurance program, Medi-Cal, which typically pays nurses less than private insurance.
“It’s worse than ever, it really is,” said Dean Chalios, president and chief executive officer of the California Association for Health Services at Home.
To solve the issue, the association is calling on California’s governor and legislature to increase Medi-Cal reimbursement rates for home nurses by 40% in next fiscal year’s budget. Chalios said a rate increase would make pay for home nursing more competitive and attract people back to the field. It would also save the government money, he said, by keeping medically fragile children out of hospitals and nursing facilities. Both are more expensive than caring for children at home.
“Even with the economic downturn, now’s really the time to do it because it’s going to save Medi-Cal money in the long run,” he said. “This needs to be done. … These children need this help, these families need this help.”
Parents of children with special health care needs interviewed by the California Health Report agreed that pay rates for home nurses need to go up—some had themselves lost nurses to higher paying positions or jobs with better benefits. A few parents offered other suggestions too, such as providing more stable hours and benefits for home nurses employed through nursing agencies, offering more home nurse training at nursing schools, and making it easier for parents to obtain nursing qualifications themselves.

Families on Their Own
Without home nursing support, families can struggle to care for medically fragile children. Some children, like Mila, stay in the hospital longer than necessary or are sent to pediatric nursing homes, said Jerin Johnson with the nursing agency Aveanna. Parents intent on having their children at home often quit work to become full-time caregivers, placing economic strain on the family. They go without sleep because children who depend on medical equipment to stay alive often require overnight monitoring. To get a break, parents may turn to relatives or babysitters without medical training.
Children enrolled in Medi-Cal are entitled by law to receive the nursing hours approved for them. The same is true for children in the California Children’s Services (CCS) program, a state insurance program for children with specific chronic conditions who require intensive levels of care. Most children enrolled in CCS are also enrolled in Medi-Cal, although some higher-income families qualify only for CCS. Nursing reimbursement rates are the same for both programs.
Since children enrolled in Medi-Cal are disproportionately low-income children of color, the difficulty in securing needed nursing care can exacerbate existing inequalities for them and their families. While wealthier families are more likely to have private insurance or can afford to pay out-of-pocket for home care, families with Medi-Cal are often left with very few options and have to fend for themselves.

Ambere Suarez of Palmdale is authorized by the CCS program and Medi-Cal to get round-the-clock nursing care for her 4-year-old daughter, Mia, who has severe cerebral palsy, is fed through a tube, is ventilator dependent, and has a tracheotomy. But since the pandemic, Suarez said she’s only been able to get a nurse for 14 hours on weekdays and eight hours on weekends, and even that is inconsistent. She said some nurses regularly come in late, call off work at the last minute, or fail to show up. Some have left for higher-paying jobs. Suarez has to fill in the gaps—including supervising Mia on her ventilator overnight—while also caring for Mia’s two sisters, ages 4 and 13.
“I’m expected to stay up and watch my child, and then take my children to school,” she said. “I’m expected to be this super mom when it’s impossible.”
Suarez said she’s had to keep her oldest daughter home from school multiple times because she’s too tired to drive. The exhaustion has led to parenting stress and disagreements with her husband, who helps with the kids on weekends but works full time to support the family. She said she’s also developed depression because of the stress.
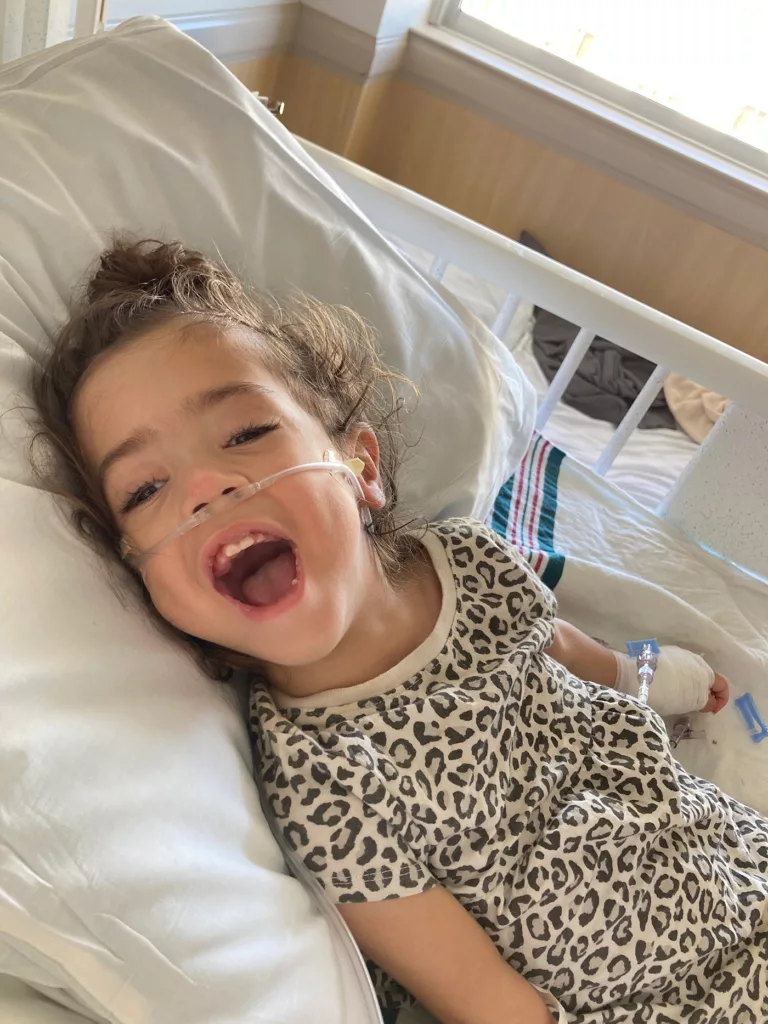
As for the Brokloffs, after failing to find a nurse for Mila, they decided to bring their daughter home from the hospital anyway. Jared Brokloff works full time, so it’s Analicia Brokloff’s job to care for Mila and the couple’s 8-month-old daughter. Analicia got training at the hospital on how to care for Mila. But she still feels nervous managing her daughter’s health condition without any nursing backup. Mila’s grandmother helps, but she also has no medical background. In fact, Analicia had to train her, even though she doesn’t feel confident herself.
A few days after Christmas, just a month after her release from UC Davis, Mila was back in the hospital with pneumonia and sepsis. Analicia was heartbroken. She wondered if it was her fault. Did she miss a warning sign that her daughter was getting sick?
“I did my best to notice her signs,” she said. “But I can’t help thinking if I had a nurse here that’s a little bit more experienced than I was, would I have caught it sooner?”

Majority of Requests Go Unfilled
Without enough nurses, home health agencies are turning away large numbers of Medi-Cal patients. Based on surveys of its members, the California Association for Health Services at Home estimates that only about 30% of home nursing hours authorized by Medi-Cal for medically fragile children are being filled. At some agencies, the shortfall is even greater. One agency in suburban Los Angeles told the association it turned away 99% of Medi-Cal referrals, while another had 366 fragile patients on its waitlist. Some agencies have lost more than half of their nurses, the association said.
Aveanna, which serves special needs children throughout California, has over 200 Medi-Cal patients on its waiting list, said Johnson, the agency’s West Region president. And so few nurses are willing to accept Medi-Cal pay rates that many children on the list may never get a nurse, she added. Waiting lists are shorter for patients with private insurance or who can pay out of pocket. Private health insurance can pay as much as 200% of the Medi-Cal rate.
“We’re just seeing a really significant social impact on (children and) the families and impact to their health,” Johnson said. “They’re not getting the care they need to stay at home, healthy, and out of the hospital.”
Johnson and Mike Beams, regional vice president of the nursing agency Maxim Healthcare Services, agreed Medi-Cal rates need to change. Current rates for home nurses range from between $19 and $45 an hour to $28 and $68 an hour, depending on the type of nursing provided and experience level (a portion of this rate is usually absorbed by the nursing agency). The state did increase rates by 50% in 2018, but that was after 15 years of stagnation and has not been enough to account for the effects of inflation, agencies said. Beams said California’s rates are now lower than surrounding states like Arizona, Nevada, and New Mexico.
“With rates being stagnant, we haven’t been able to increase pay rates to keep up with rising costs of living anywhere in California,” he said in an email. “This has caused us to lose longtime staff who have been with patients for years and forced us to focus our limited recruitment resources on backfilling current positions.”

Lori Ann Dotson, who lives in San Diego County and has worked in the disability field for decades, said other changes are needed too. Dotson is mother of a 9-year-old daughter with severe disabilities and has also struggled to get nursing care, even though she and her husband have private insurance in addition to Medi-Cal.
Dotson said nursing schools need to introduce more students to the home nursing field and help build up the home care workforce. She suggested pay rates for home nurses be similar, regardless of whether they’re a licensed vocational nurse or a registered nurse. The current structure, which reimburses more for registered nurses because they have more training, incentivizes agencies to hire these nurses over licensed vocational nurses, even though both can do home nursing, Dotson said. Additionally, home nurses should be given more opportunities for advancement and more stable pay and benefits to make it a more attractive career, she said.
Analicia Brokloff, meanwhile, has come up with her own solution. She’s studying to become a nurse herself so she can get hired through an agency to care for her daughter. She recently started a four-week nursing assistant program and plans to train as a licensed vocational nurse after that. Eventually, she hopes to become a registered nurse, which would take about two years. Her mom watches Mila while she’s in class.

“If I can’t find a nurse, I’ll just be nurse,” she said. “That’s kind of the only option that we’re left with.”
She worries about other families of children with disabilities that don’t earn enough to have one parent stay home, or to even think about pursuing a nursing qualification.
“It just makes me sad,” she said. “We’re trying to get this help and we’re going to these lengths to make sure that our kids are happy, but it’s not manageable right now, it’s really not.”
This story was produced in partnership with the California Health Report.

|
Claudia Boyd-Barrett
is a longtime journalist based in southern California. She writes on topics related to health care, social justice, and maternal and child well-being. Her investigative stories on access to mental health care have resulted in legislative and policy changes.
|


