News Based on facts, either observed and verified directly by the reporter, or reported and verified from knowledgeable sources.
A Day in the Life of Parents Caring for a Child With Complex Medical Needs

It’s still dark when Claire Hernandez has her first meal of the day. In fact, the 3-year-old is often still sleeping. Her father, John Hernandez, tiptoes into her nursery and, gently, so as not to wake her, attaches a feeding tube to her stomach. The vitamins and medications that flow through the tube help Claire, who has a rare genetic condition, survive. So does the love and dedication of her parents. Without their commitment and round-the-clock care, Claire would live in a hospital or institution, or possibly, tragically, not be here at all.
As her parents see it, caring for Claire is part of the job of being parents and something they do gladly, just as they care for her older brother, 7-year-old Xavier. Claire was born, apparently healthy, in December 2021 in Los Angeles, where the family still lives. Her parents never anticipated that four months later, after having brain swelling and open-heart surgery, their infant would be diagnosed with a condition so rare that only 20 people have been known to have it. Or that it would mean Claire’s mother, Vivian Vasquez, would become Claire’s full-time caregiver, and lose her job as a high school principal in the process, that the family would burn through their savings and need public assistance for health care, that they’d have to battle endless insurance program denials and paperwork to get care that doctors said Claire needed. Perhaps most shocking was that the health and social support system that’s supposed to help families like Claire’s would, instead, make it even more stressful to care for a child with intensive medical needs.
“When you are trying to care for a human baby and all you find are walls … it’s this stone-cold feeling,” Vasquez says. “How do I find the help I need? There’s no one to direct you.”
If Vasquez, who holds two master’s degrees, has struggled to figure out how to get health coverage and care for Claire, what happens to other, less-resourced families? California has multiple programs that provide support to children with complex medical needs and disabilities. Among them are Medi-Cal, the state’s safety-net health insurance program; a waiver program that allows kids with disabilities to qualify for Medi-Cal even if their parents earn too much; California Children’s Services, which provides treatment for children with certain medical conditions; In Home Supportive Services, which pays for caregiving of people with disabilities at home; and California’s Regional Center system, which serves kids and adults with developmental delays.
But accessing and making use of these programs is a minefield for many families. They often receive little guidance on how to apply for programs, must navigate complex paperwork and bureaucratic requirements, wait weeks or months to find out if they’re approved for a service, and—then, even if they do qualify—struggle to find providers that can offer the sanctioned care. The result is that children often don’t receive the care they need—which can lead to a need for even more care as they get older and increases the risk of the child requiring expensive visits to hospital emergency rooms. Some parents give up on trying to get services altogether and become emotionally or financially distressed. It’s common for at least one parent to have to stay home to care for the child, affecting the family’s income.

“I Can See Where People Would Give Up”
Claire is a vivacious child, with attentive brown eyes and the round cheeks of a toddler. Although she can’t talk, she babbles constantly, and flashes smiles at strangers and family members alike.
Born with a rare genetic condition that affects her heart, lungs, and brain function, Claire’s survival depends on a strict routine of alternating feeding, breathing, and medication treatments. These continue from the moment she wakes up until her bedtime around 9:30 p.m., when she sleeps attached to an oxygen machine.
An hour after Hernandez has given Claire her first supplements every morning, Vasquez steps into the little girl’s nursery.
“Hi, Claire bear,” Vasquez says. “Good morning, little honeybun.”
If she’s not too tired, the toddler stretches and greets her mom with a big smile. Vasquez props Claire up in bed or on the couch in the living room. She turns on The Wiggles—a children’s music show—on a tablet and uses a syringe to give her daughter the first of six meals of the day through her feeding tube. Claire likes to move along to the music and point and flex her toes when her favorite ballerina song comes on.
After making Xavier breakfast and driving him to school, Vasquez continues Claire’s feeding and treatment routine for the rest of the day and works with her on exercises to help physical and mental development, such as standing her against the wall, holding her head up, and putting toys in front of her. She balances this with taking Xavier to kung fu or piano lessons in the afternoon and helping him with homework.
But that’s just part of her responsibilities.
The stack of manila folders on the kitchen table is another story. Inside are papers related to health insurance programs, medical services, and social assistance Vasquez has sought to try to get Claire’s needs met and support her family financially.
“Everywhere I go, there’s something else to apply for,” Vasquez says, estimating that she spends two hours a day calling government agencies, health insurance officials, and doctor’s offices, often with little success. “I know the help is out there, it’s just hard to access it. … I can see where people would give up.”
“We have a very complex health care system,” says Apple Sepulveda, an occupational therapist with the Nurture Collective in Los Angeles, who specializes in working with young children who have medically complex conditions, and is helping to teach Claire how to swallow. She says she’s constantly meeting parents like Vasquez who are struggling to get the support their child is entitled to, while trying to cope with the upheaval of caring for a child with intensive health needs. Because they don’t get enough help, parents can become overwhelmed or depressed, she says.
“Navigating all these services and appointments is time-consuming for families,” Sepulveda says. “We have to recognize that a lot of these parents are so overwhelmed because they bring their child home from the hospital or the NICU and they become their nurse, their care navigators, their advocates, their respiratory therapists. So, they wear a lot of hats.”
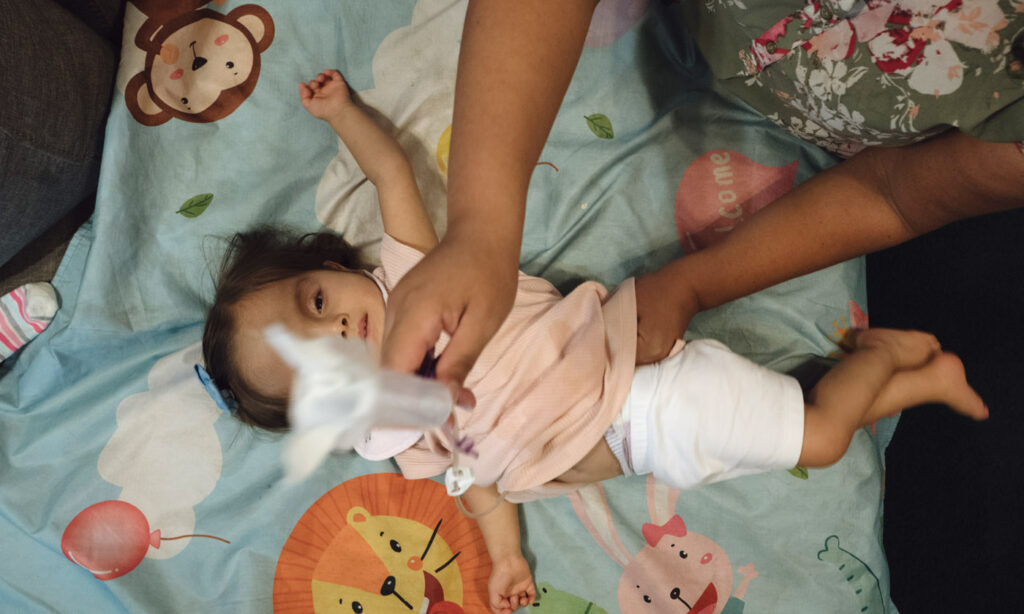
The Impact of Delays
Claire had open-heart surgery at 4 months old and shortly after was diagnosed with “chromosome deletion 4q21q22.” The condition impairs the body’s organs, delays growth, and affects feeding, speech, and mobility. Vasquez remembers how sad she felt when the doctors sat her and Hernandez down in a hospital office and told them that Claire might never walk or learn to speak. Vasquez’s dreams of taking her daughter to dance class and teaching her to read shattered. She wondered if Claire would ever learn to run, if she’d ever hold a balloon.
The doctors said Claire needed regular care from multiple specialists, occupational and speech therapy, tube feedings with specialized food, and oxygen equipment to help her breathe.
She also needed more health insurance.
At the time, Vasquez was principal of an elementary school in Pomona, the culmination of a long career of teaching, founding a bilingual education program, and earning two bachelor’s and two master’s degrees. She had private health insurance for her family through her employer. But that insurance wasn’t enough to cover all the complex care that Claire required. Vasquez also needed a home nurse to care for Claire during the day while she worked. Although she and her husband made enough to live comfortably, these expenses were more than the family could afford. They also had a mortgage to pay, student loans, and two car loans, and were helping Vasquez’s elderly parents with utility bills.
At first, Vasquez thought she had it figured out. A hospital social worker recommended she apply for the Medi-Cal and Home and Community-Base Alternatives (HCBA) waiver programs, which would cover Claire’s medical care. She also learned that, once Claire had Medi-Cal, she could apply for the state program that pays for a home nurse.
But it took months to get approved. First, Vasquez applied for standard Medi-Cal in June 2022, but was denied because her family’s income was too high. Then she applied for the waiver program, the other avenue to Medi-Cal coverage, which required gathering mountains of evidence for Claire’s condition. She waited three months for that to be approved. Then, upon receiving the approval, Vasquez had to reapply for Medi-Cal to get actual health coverage, which took effect in January 2023. Because of the delay in getting insurance, during the eight-month process to obtain Medi-Cal Claire hadn’t seen most of the specialists she was entitled to see under federal health care law, which requires that children enrolled in the safety-net health insurance program receive all medically necessary treatment.
Eight months is a long time when you are a toddler. It amounted to nearly half of Claire’s life that she had gone without the health care doctors said she needed. Early intervention is critically important for many children’s health and developmental conditions, increasing the likelihood that treatment will work.
Only when Claire had Medi-Cal could Vasquez apply for the home nurse program. Again, Vasquez waited about nine months for the application to be finalized. Eventually, she called the program’s customer service line in frustration, dialed through multiple prompts and waited two hours for someone to answer. She was told a form she had handed in was missing. It wasn’t until September that she received the first home nursing payment.
By that time, Vasquez had been fired from her job for missing too much work. She couldn’t juggle the demands of running a school with caring for Claire without the help of a nurse. With the loss of employment, Vasquez also lost the family’s main source of income, and her own and Xavier’s health insurance. She and Hernandez, whose job doesn’t offer family health coverage, began burning through their savings to stay afloat.
“I’ve never felt the amount of stress in my life as I have these last two years,” Vasquez says. “It just all crumbled down … I’ve had to reprioritize, readjust our lives.”
Ironically, Vasquez’s newly precarious financial situation made her and Xavier eligible for Medi-Cal. That application process took another three months, forcing Vasquez to burn through even more savings to pay for out-of-pocket medical bills for her and Xavier while she waited for their Medi-Cal cards.
“We didn’t qualify for Medi-Cal at first because we earned too much,” she noted. “It’s like you have to be reduced to low-income to get the help you need.”
All in all, the process of getting Claire the care she is entitled to—and needs—and health coverage for the rest of the family has taken more than a year and a half. And it’s not over yet. Vasquez is still trying to secure appointments with a developmental neurologist and speech therapist for Claire, and is trying to figure out how to apply for California Children Services, which she hopes will help cover some of the treatment.

“A Cloud Above My Head”
The Vasquez family’s worries didn’t end when they were finally enrolled in Medi-Cal and In Home Supportive Services, the home nursing program. Vasquez is compensated by Supportive Services for some of her caregiving hours, but at $17 an hour it’s only about half of her previous salary, and barely above minimum wage. Meanwhile, with Claire enrolled in Medi-Cal under the Home and Community-Based Alternatives waiver, Vasquez has struggled to find new specialists that take the insurance and don’t have a long waiting list.
Almost a year since having Medi-Cal, Vasquez is still working to get Claire all the doctor’s appointments and therapies she’s been told she needs. Provider shortages, particularly among those that accept Medi-Cal, make finding pediatric specialists difficult. And the doctors Vasquez used under her private plan don’t take Medi-Cal. Many doctors don’t accept Medi-Cal because it offers them a lower pay rate than private insurance, resulting in a tiered health care system that further exacerbates health disparities for Californians.
Claire’s Medi-Cal plan sent referrals to at least 11 specialists, but most of them weren’t taking appointments for months and still had to get final approval from Medi-Cal before they could see Claire. Vasquez had to pester them to try to ensure the referrals and approvals went through. This meant waiting months to see a primary-care physician, a pulmonologist, gastroenterologist, cardiologist, and other specialists. She’s still waiting for calls back for a developmental neurologist.
She’s also spent months fighting to get occupational and physical therapy, and now speech therapy for Claire. Vasquez applied for these services through the Eastern Los Angeles Regional Center in June 2022, but says she’s faced an uphill battle getting the therapies fully covered. She’s had to put in multiple requests to prove she couldn’t get coverage through her old health plan. Claire now has occupational and physical therapy twice a week, but Vasquez is frustrated that it took so long to get it. The Regional Center still hasn’t approved speech therapy, even though multiple providers have said Claire needs it. Vasquez is worried that the difficulty in getting these therapies and speech intervention has put her daughter’s development further behind.
To add to her to-do list, Vasquez now has to reapply for Claire’s Medi-Cal and HCBA waiver, because California has restarted its renewal process for health benefits after ending a three-year pause during the pandemic.
“When I think of the system, I feel like it’s just me and this cloud above my head with all these acronyms and bureaucracies and buildings and I’m like, ‘OK, which of them am I reaching for today?’” she says. “I’ve learned to take it one day at a time.”
Sepulveda says California needs to make it easier for families like Vasquez to get services. A new service under Medi-Cal called Enhanced Care Management that would provide care coordination for children like Claire could help, she says, but the benefit has been slow to rollout and many people are skeptical it will work. Vasquez says what she really needs is someone to walk through the system with her and provide ongoing support, rather than leaving her to figure everything out for herself. She wants it to be easy to call and get help, and to feel that those who answer the phone recognize her and her daughter as human beings, not just numbers and checkboxes.

Claire, meanwhile, is growing and gaining new skills, on her own timetable. She babbles, rolls over, and can pick up small items with her fingers like her pacifier and crackers. She recognizes people and smiles. The biggest smiles are for Vasquez, Hernandez, and Xavier.
But Claire doesn’t yet sit unassisted, crawl, or walk, as typically developing 3-year-olds would, and she hasn’t learned to speak.
Vasquez is holding out hope that Claire will eventually learn to do all these things. She dreams of using her education skills to one day teach her daughter to read. For now, she celebrates each small achievement, marveling at Claire’s determination.
“No one ever thinks they’re going to have a child with a condition,” Vasquez says. “It really does shatter hopes, but in a way it’s actually made me stronger. She’s taught me so much about what real courage is and what real beauty is. “
Sometimes, Vasquez and Hernandez get out the photo of Claire after her heart surgery at 4 months old, her tiny body covered in tape and stitches, her little face intent on breathing, on staying alive. She has done it. She is still doing it.
And her parents are helping her every step of the way.
This story was produced in collaboration with the California Health Report.

|
Claudia Boyd-Barrett
is a longtime journalist based in southern California. She writes on topics related to health care, social justice, and maternal and child well-being. Her investigative stories on access to mental health care have resulted in legislative and policy changes.
|

|
Hannah Hough
is the executive editor of the California Health Report, which partners with communities across the state to share ideas for making our world more equitable. She speaks English, and is a member of INN and LION.
|






